Age-related macular degeneration (AMD) is one of the leading causes of permanent vision loss in adults over 65. If you or someone you care about has been diagnosed with AMD, or if a doctor has mentioned it as a concern, you’ve likely heard the terms “wet” and “dry” used to describe it. These refer to two distinct forms of the disease with different symptoms and treatment paths. Knowing the difference can help you ask the right questions and make informed decisions about your eye health.
What Is the Macula, and Why Does It Matter?
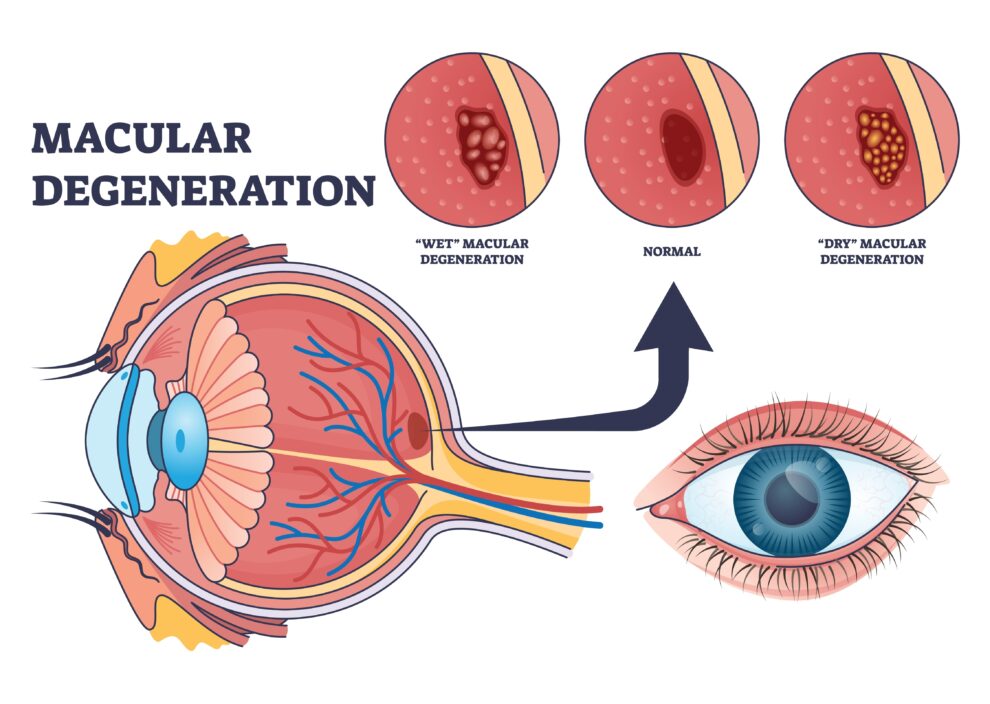
To understand AMD, it helps to know what the macula does.
The macula is the small, central region of the retina responsible for your sharpest, most detailed vision. It’s what allows you to read, recognize faces, drive, and focus on anything directly in front of you. When the macula begins to deteriorate, that central field of vision becomes blurry, distorted, or dark, while peripheral vision often remains intact. Macular degeneration damages this part of the retina and is often age-related.
Dry Macular Degeneration: The More Common Form
Dry AMD accounts for the vast majority of all AMD cases. It develops when the light-sensitive cells in the macula gradually break down over time, typically as a result of aging.
The earliest and most recognizable sign is the buildup of small yellowish deposits beneath the retina called drusen. Nearly everyone develops some drusen with age, but larger or more numerous deposits are closely tied to the degeneration of cells in the macula.
Dry AMD progresses through three stages.
In the early stage, drusen are present, but vision may appear normal.
At the intermediate stage, larger drusen have accumulated, and mild blurriness or difficulty seeing in low light may develop.
In late-stage dry AMD, a condition called geographic atrophy, cells in the macula have died off in patches, leading to significant central vision loss.
One of the defining features of dry AMD is how slowly it progresses. Vision changes may be so gradual that patients don’t notice them for months or years.
Wet Macular Degeneration: Less Common but More Aggressive

Wet AMD, also called neovascular AMD, accounts for a smaller percentage of cases, but it is responsible for the majority of severe, rapid vision loss associated with the condition.
It occurs when abnormal blood vessels grow beneath the retina in a process called choroidal neovascularization. These new vessels are fragile and prone to leaking fluid or blood directly into the macula, which is what gives wet AMD its name.
The damage caused by leaking vessels can be swift and severe. Where dry AMD might take years to meaningfully affect vision, wet AMD can cause noticeable changes in a matter of weeks.
Patients often report that straight lines appear wavy or bent, a symptom called metamorphopsia, or notice a sudden blurry or blind spot near the center of their vision. Some describe colors as appearing less vivid or washed out. Any sudden change in central vision should be treated as an urgent reason to see an eye doctor.
Wet AMD almost always develops in eyes that already have dry AMD. Dry AMD does not inevitably convert to wet AMD, but the risk increases with advancing disease stage. This is one reason that ongoing monitoring matters even when vision remains stable.
What Are the Treatment Options?
For dry AMD, the primary strategy is monitoring and risk reduction. The AREDS2 supplement formula, a specific combination of vitamins C and E, lutein, zeaxanthin, and zinc, has been shown to reduce the risk of progression to advanced AMD in eligible patients. Lifestyle modifications such as not smoking, maintaining cardiovascular health, and protecting eyes from UV exposure may also play a role in slowing the disease.
For wet AMD, anti-VEGF injections are the standard of care. These medications, administered directly into the eye, block the growth factor that drives abnormal blood vessel formation. When started early, anti-VEGF therapy can stabilize vision and, in many cases, produce meaningful improvement. Laser-based treatments may also be considered in select cases.
Early detection is critical for both forms. The team at Whitson Vision uses the AdaptDx® imaging test, one of the most accurate tools available for detecting the earliest signs of AMD before symptoms appear. This technology measures dark adaptation, the eye’s ability to adjust from light to dark, which is one of the earliest functions to decline as AMD develops.
When Should You Get Checked?
Several factors raise the likelihood of developing AMD. Age is the most significant, with adults 65 and older at the highest risk.
A family history of macular degeneration, a history of smoking, high blood pressure, and prolonged UV exposure without eye protection are all contributing factors. AMD also tends to affect both eyes, though one eye may show more advanced disease than the other.
Because early AMD often causes no symptoms, many patients are unaware they have it until the disease has progressed. A comprehensive eye exam that includes a dilated retinal evaluation is the most reliable way to detect AMD at a stage when intervention is most effective.
AMD is far from the only condition that progresses silently. Glaucoma and diabetic eye disease follow the same pattern, reinforcing why annual exams matter more as you age.
If you’ve noticed changes in your central vision, or if you’re over 65 and haven’t had a dilated eye exam recently, don’t wait. Schedule an appointment at Whitson Vision in Indianapolis, IN, today!